Stress is ubiquitous in our modern lives. Everyone is suffering from ‘stress’. But not many people actually understand what it means, or about the long-term negative effects it can have on the body.
The fight or flight response, the sympathetic nervous system and the adrenal glands
To understand the impact of stress, we first need to understand about the fight or flight response and the systems it activates. This is our bodies primitive, automatic and innate response that enables us to ‘fight’ or ’flee’ from perceived attack or threats. Its sole purpose is ensuring we’re able to survive by redirecting all our energy to the systems that give us the physical capabilities to literally run or fight for our lives. The response is hardwired into our brains: it developed over millions of years of evolution from our prehistoric ancestors to our current physiology to ensure our survival from the threats we faced at that time. The process occurs within a millisecond of our brain registering stress. Perception of stress by the brain results in the activation of the stress response via two complementary mechanisms: the hypothalamic-pituitary-adrenal (HPA) axis and the sympathetic nervous system (SNS), both of which communicate with a pair of glands that sit above your kidneys called your adrenals, which pump out different stress hormones as a result of each system-
- SNS – a short-term stress response where the brain tells the adrenal glands to release noradrenaline and adrenaline. This is immediate, as it occurs via lightning-quick nerve signals, and is designed to give short bursts in energy and attention while we’re waiting for the next system to kick in.
- HPA Axis- a more long-term stress response that involves the brain telling the adrenal glands to release a hormone called cortisol. This is slightly slower, as it involves 2 separate structures in the brain (the hypothalamus and the pituitary gland) communicating with each other before then releasing a hormone that has to travel by the blood to the adrenals to tell them to activate. The adrenal glands of a healthy person produce about 20mg of cortisol each day, but this can increase to 200mg a day during periods of stress.

Normal cortisol levels are necessary for maintaining blood sugar, promoting anti-inflammatory actions, controlling our immune cells, regulating blood pressure, as well as influencing the central nervous system controlling mood and behaviour. And while transient spikes in cortisol and adrenaline are meant to provide burst of energy, chronic activation of the stress response is dangerous because of the impact these hormones have on the body if their release is sustained. Within one week of continued stress, we start to see detrimental physical changes. The body starts to alter its processes in an attempt to protect itself, and it’s the outcome of these alterations that we perceive when we have “adrenal fatigue”. This is an old-fashioned term that was originally coined because it was thought the adrenals “fatigued” after being activated for a sustained period and shut down. But in actual fact, the entire HPA axis is downregulated (i.e., the brain no longer asks the adrenals to produce cortisol) as an adaptive protective response, which is why adrenal fatigue is now called HPA axis dysfunction.
What causes HPA dysfunction
Unfortunately, our primitive brain can’t differentiate between the stress of being attacked by a wild animal and that of being stuck in traffic when you’re already running late. As a consequence, our bodies are under a constant barrage of chronic stress, and it’s this chronic perceived stress that is the biggest driver of HPA dysfunction.
Other causes include blood glucose dysregulation, chronic inflammation (consider your gut, allergies, musculoskeletal issues and obesity) and imbalances to circadian rhythm (e.g., shift work, travel… not so much the last one right now).
How can we check where your stress levels are at?
One of the best ways to assess your stress levels is with a salivary cortisol test: by collecting and analysing the cortisol levels in your saliva throughout the day we are able to see how your HPA axis and stress response are travelling. Depending on the shape of the curve we can determine if you’re in the early stages of HPA dysfunction (with high cortisol levels throughout the day – think “wired and tired”) or later stages (with low levels and a flat curve – think “flat and exhausted”), and then tailor your treatment accordingly. If you’re sleeping poorly, we can also check your cortisol and melatonin throughout the night to see if your stress response is impacting your sleeping patterns.
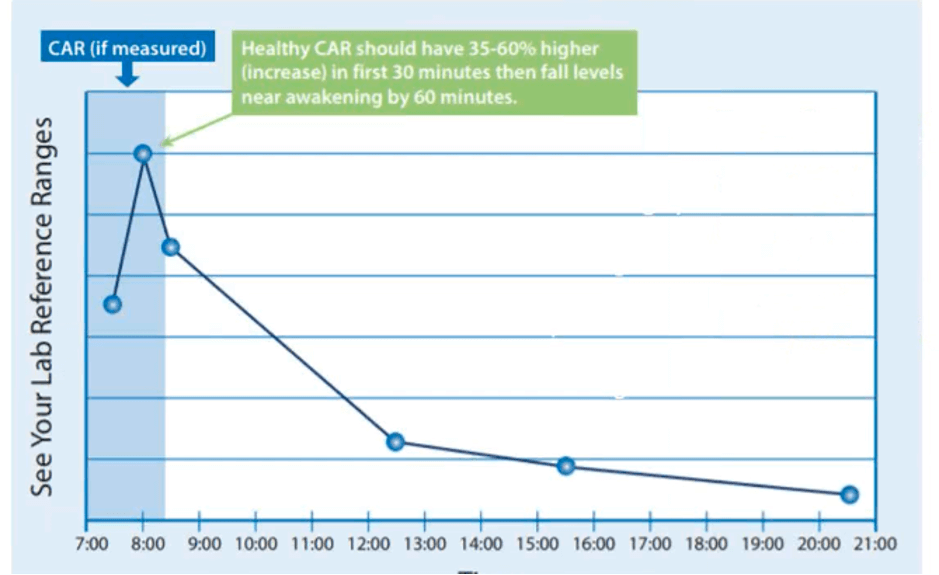
Another option we can look at is your cortisol awakening response (CAR). This is another saliva test that looks specifically at your cortisol levels in the first 2 hours of waking. Normally in the first 30 minutes of waking there should be a big spike in cortisol production, lifting anywhere from 35-60%, after which it drops off. This spike is crucial, because it actually sets up the cortisol production for the rest of the day, so this test can help us understand why your cortisol patterns may be suboptimal throughout the rest of the day.
If the CAR spikes too high it’s usually because someone is suffering anticipatory stress about the coming day, and often sees them experiencing anxiety the rest of the day. If it doesn’t spike at all (or even drops) it’s usually because someone is not sleeping properly or has end stage HPA dysfunction, and they usually feeling really groggy (they’re the ones who need 3 cups of coffee to get their eyes open).
Whichever patten of HPA dysfunction you’re experiencing, there are specific herbs, nutrients and lifestyle recommendations that can help you restore your stress response and have the energy to thrive again.
Get in touch with Ali Berecry, Naturopath at pH clinic if you would like more information, or please make a booking here.



